Category: “Accountable Care Organizations”
- CMS: Medicare ACOs continue to succeed in improving care, lowering cost growth
- U.S. patients of Accountable Care Organizations (ACOs) to exceed 130 million by 2017
"The digital health markets need to develop business models that make sense while organizations are transitioning to these different care reimbursement models," said Sandra Elliott, Director, Consumer Technology and Service Development, Meridian Health. "Health and technology providers should focus on providing end-to-end scalable solutions that offer financial benefits to purchasers while showing value to patients as individuals by enabling them to live their life to the fullest, thus encouraging strong consumer engagement."
- IDN update – many are becoming insurance providers as well as care
The need to form ACOs and cut costs has also resulted in IDNs wanting to provide more than healthcare - they want to be the insurer as well. What does it mean when one organization controls both the insurance side and the delivery side of the business?
- ACOs: A Step in the Right Direction
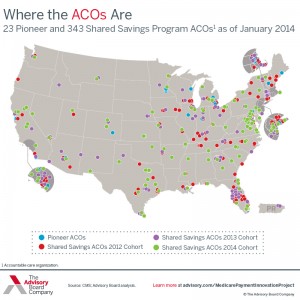
- Learn the state of ACOs by the numbers
- ‘Obamacare’ Is More Than Exchanges
Important charts and information on Medicare Expansion, ACO locations, and readmission rates across the US
- Hospital consolidation generally results in higher prices.
The Patient Protection and Affordable Care Act (ACA) promotes Accountable Care Organizations (ACOs) and the bundling of payments across providers for an episode of care (“bundled payments”), both of which encourage consolidation between hospitals and physician practices.
- Sharp HealthCare ACO drops out of Medicare’s Pioneer program
- ACO directory: 272 ACOs in America
- The Role of Pharmacy Care is a Blind Spot in ACOs
- NYT – ACOs and Mergers might be good for business but not so much for patients
Larger organizations have greater market power to demand higher prices from those plans for doctor visits and hospital stays. And higher prices paid by plans translate into higher premiums for consumers.
- Inside Obamacare – Forbes primer on the ACA law and how it impacts US Healthcare
- Radiology Prepares for the ACA, Including a Potential Flood of Patients
In retrospect how wrong they were...
- Six Wisconsin systems create pact, aim for ACO
The six systems are Aspirus in Wausau; Aurora Health Care in Milwaukee; Bellin Health in Green Bay; Gundersen Health System in La Crosse; ThedaCare in Appleton; and UW Health in Madison. Together, they comprise 44 hospitals and more than 5,600 physicians, and they provide care to about 90% of the Badger State's population, according to a release announcing the partnership.
Matt Heywood, CEO of Aspirus, said in an interview that the ultimate goal of the non-equity partnership is to migrate toward an accountable care organization. The six health systems already have started offering a commercial health plan with Anthem Blue Cross, available through the federal and private-insurance exchanges. If and when the collaborative becomes an ACO, it will aim for inclusion in more health plans as a low-cost, high-quality provider network.
- 70 Accountable Care Agreements Announced So Far This Year
- 3 Ways to Improve the ACO Model
- ‘Value-Based’ Contracts To Hurt Profits
- The AHA says the financial risks of ACO participation outweigh the rewards
- Almost 30% of ACO Pioneers dropping out of the program